Images chosen by Narwhal Cronkite
Syringe Reuse at Pakistan Hospital Infects 331 Children with HIV: A Crisis Rooted in Neglect
Inside a crowded hospital in Pakistan’s Punjab province, a horrifying pattern of unsafe medical practices has emerged, leaving behind a trail of heartbreak and tragedy for hundreds of families. According to an investigation conducted by the BBC, the reuse of syringes at Taunsa’s THQ Hospital has resulted in 331 children testing positive for HIV, a grim finding that exposes systemic lapses in infection control and healthcare oversight.
The consequences of these actions—or inactions—are devastating. Eight-year-old Mohammed Amin’s death, shortly after being diagnosed with HIV, draws a painful spotlight on the ripple effects of negligence. His sister Asma, also infected, stands as another testament to the unquestionable need for urgent healthcare reform in Pakistan. The story of Taunsa is not simply a local tale of malpractice; it is a cautionary tale with international implications for public health systems worldwide.

The Investigation: Widespread Negligence Captured on Film
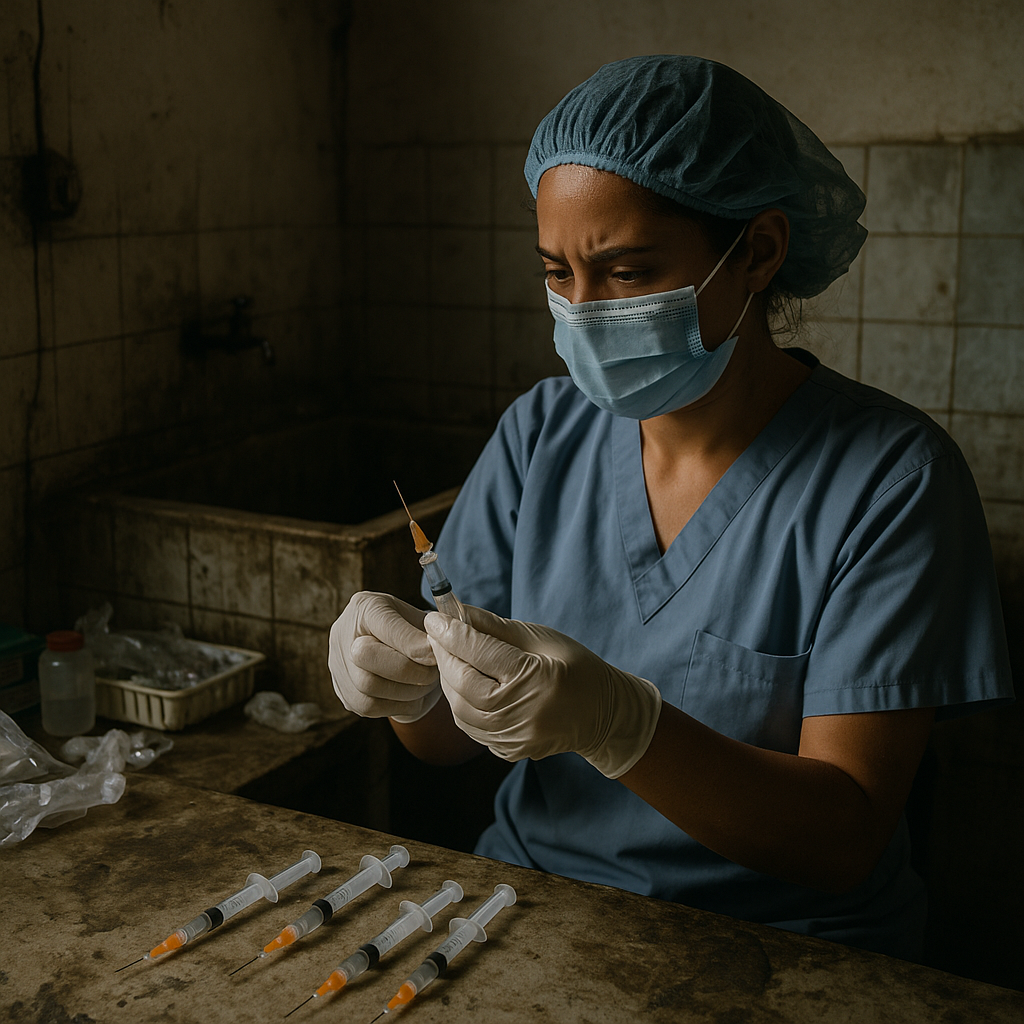
The BBC investigation brought to light 32 harrowing hours of undercover footage captured inside the THQ Hospital in Taunsa. This footage revealed repeated violations of basic hygiene protocols, including the reuse of syringes across multiple patients. Nurses and staff were seen drawing medication from multi-use vials using contaminated syringes, a practice that exponentially increases the risk of cross-contamination.
“Even if a new needle is attached, the syringe body can carry the virus,” explained Dr. Altaf Ahmed, a consultant microbiologist, highlighting the grave risks posed by these practices. Despite clear video evidence, hospital administrators have denied any wrongdoing, a stance that only deepens the frustration and distrust among families of the affected children.
Data compiled from provincial healthcare screenings and leaked police records between November 2024 and October 2025 identified 331 confirmed pediatric HIV cases in Taunsa. In more than half of these cases, unsafe injections were cited as the likely transmission pathway. Alarmingly, maternal transmission—a more common cause of pediatric HIV globally—was ruled out for most cases as only 4 out of 97 tested mothers were HIV-positive.
A Healthcare System Under Strain
The situation in Taunsa underscores the fragility of Pakistan’s healthcare system, particularly in rural and underserved areas. For years, public health experts have raised alarms about inadequate training, lack of accountability, and chronic resource shortages in government hospitals across the country. These systemic issues, coupled with insufficient regulation and oversight, create an environment where shortcuts and unsafe practices can flourish unchecked.
According to Dr. Gul Qaisrani, the local physician who first noticed the unusual rise in pediatric HIV cases, the issue isn’t just about individual negligence but a breakdown of the entire healthcare infrastructure. “When doctors and nurses work in overcrowded conditions without basic supplies, the temptation to cut corners becomes dangerously real,” Qaisrani stated.
Pakistan’s healthcare expenditure, measured as a percentage of its GDP, remains among the lowest in the region. This chronic underfunding translates to outdated medical equipment, insufficient staff-to-patient ratios, and inadequate infection control training—all of which set the stage for preventable tragedies like the one unfolding in Taunsa.
Public Trust: The Collateral Damage
Beyond the immediate public health toll, the broader implications of the Taunsa outbreak extend to public trust—a critical component of any successful healthcare system. Parents in the region now face a painful dilemma: do they seek medical care for their children but risk infection, or avoid hospitals altogether, allowing treatable conditions to worsen unchecked?
Community members expressed outrage and despair following the revelations. “How can we trust these institutions to heal us when they are the same places causing harm?” one father lamented outside the hospital where his son had been treated. The loss of trust extends to healthcare workers as well, many of whom rely on this profession to safeguard not only their livelihood but also their identities as caregivers.
Similar outbreaks over the past decade—such as the 2019 HIV crisis in Ratodero, Pakistan—add to the growing disenchantment with the country’s healthcare system. Industry observers have noted that without strong accountability mechanisms, the cycle of malpractice and public distrust will continue, exacerbating existing disparities in health outcomes.

Global Lessons in Patient Safety
The Taunsa outbreak raises fundamental questions that resonate far beyond Pakistan’s borders. How can public health systems—especially those in low- and middle-income countries—ensure basic safety protocols amid resource constraints? What role should international organizations play in addressing such outbreaks without impinging on national sovereignty?
The World Health Organization (WHO) has repeatedly emphasized the importance of injection safety in healthcare systems, and Pakistan’s repeated outbreaks serve as stark reminders of the consequences of ignoring these guidelines. The WHO estimates that globally, unsafe injections are responsible for up to 9 million new infections annually, spanning diseases such as HIV, Hepatitis B, and Hepatitis C.
Experts argue that Taunsa should be seen as a wake-up call for greater international cooperation in tackling systemic healthcare challenges. From funding robust training programs for healthcare workers to ensuring hospitals are equipped with adequate supplies, many believe that a collaborative effort between national governments and international health bodies is key to preventing future tragedies.
What Comes Next?
While the tragedy in Taunsa has already changed hundreds of lives irrevocably, the road to recovery and prevention remains steep. Authorities in Pakistan must act decisively to investigate and address the failings that led to this crisis, beginning with enforcing accountability for protocol violations at the THQ Hospital. Systemic reforms in infection control training, syringe disposal policies, and resource allocation should follow.
Equally important is the need for public outreach—educating communities about the risks of unsafe medical practices while rebuilding trust in healthcare institutions. Without these efforts, the scars left by the Taunsa outbreak will deepen, perpetuating cycles of fear and neglect long after the headlines fade.
As the international community watches closely, Taunsa stands as both a warning and an opportunity—exposing the fragile foundations of healthcare systems while demanding urgent, collective action to shore up their resilience. In a world where the next public health crisis may be just around the corner, the time to act is now.