Images chosen by Narwhal Cronkite
Knee Surgery for Cartilage Damage May Hurt More Than Heal, Study Reveals
If you’ve ever been told that knee surgery is the solution for lingering pain or cartilage issues, you may want to think again. A 10-year longitudinal study has delivered controversial findings: patients undergoing partial meniscectomy, one of the most common knee procedures, may fare worse in the long run compared to those who forgo the surgery entirely. With millions worldwide affected by meniscus tears, a critical re-evaluation of this treatment practice is underway.
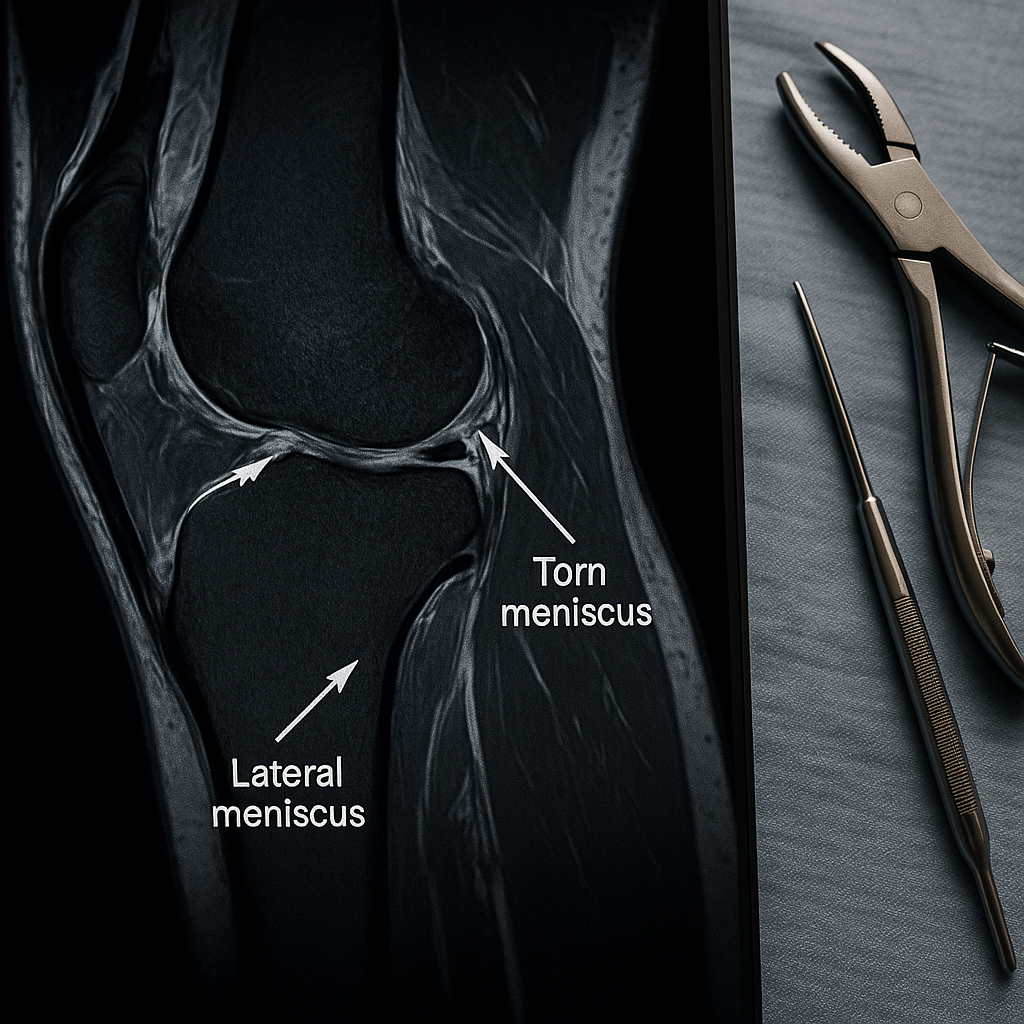
The Meniscus Dilemma: Common Surgery Under Scrutiny
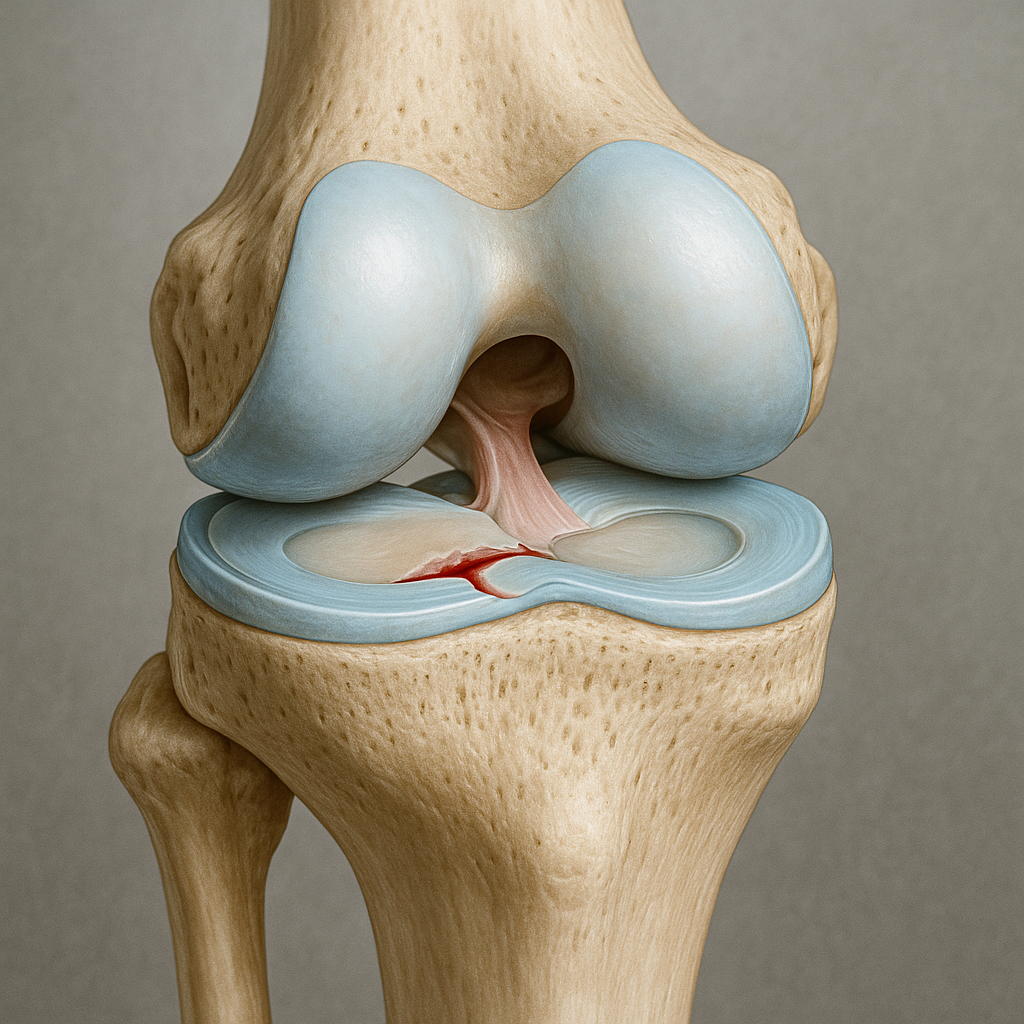
The meniscus, a C-shaped cartilage pad in the knee, acts as a vital shock absorber during movement. Tears to the meniscus occur either suddenly—often due to sports injuries—or gradually as part of the aging process. Traditionally, a meniscus tear combined with symptoms such as pain or stiffness has often led to a recommendation for partial meniscectomy, a procedure that involves surgically trimming frayed or damaged tissue.
However, the study, led by Prof. Teppo Järvinen from the University of Helsinki, casts serious doubt on this approach. It followed 146 patients, none of whom were under the age of 35, and compared those who received meniscus surgery with a control group that underwent sham surgery, where no actual procedure was performed. The results are striking: after a decade, patients who underwent the surgery reported worse knee function, higher rates of osteoarthritis progression, and more persistent pain compared to their counterparts.
This challenges the foundational belief that partial meniscectomy is an effective treatment, suggesting instead that it may contribute to further damage—a phenomenon Järvinen terms a “medical reversal.” As he explains, “Our findings suggest that this may be an example of therapy that is broadly adopted but proves ineffective or even harmful over time.”
Why the Procedure Fails the Test of Time
One of the most intriguing revelations from the study is that having a meniscal tear, in and of itself, may not always necessitate medical intervention. “We now know that these meniscal tears are very frequently found in patients with no symptoms,” Järvinen notes. Magnetic resonance imaging (MRI), a standard diagnostic tool for such injuries, often reveals tears even in healthy individuals without any noticeable knee problems.
These so-called “incidental findings” can complicate decision-making. As non-orthopaedic organizations like the UK’s National Institute for Health and Care Excellence (NICE) and the Choosing Wisely campaign have pointed out, imaging results should not automatically guide treatment. Instead, the focus should be on the patient’s symptoms and functional limitations. Over the past two decades, mounting evidence has indicated that not every tear requires invasive action, with physical therapy and conservative management increasingly favored as first-line recommendations.
Critics of partial meniscectomy argue that removing parts of the meniscus compromises the joint’s structural integrity, increasing mechanical stress on the knee. This, in turn, may speed up the degeneration of cartilage, contributing to osteoarthritis—a chronic condition that places an enormous burden on public health systems globally. According to a report on KevinMD, knee osteoarthritis already affects millions of adults, with cases expected to rise due to aging populations.
Rethinking Orthopaedic Surgery: A Changing Paradigm
The findings align with a broader shift in how orthopaedic interventions are approached. Many independent healthcare organizations, including NICE, have begun recommending against routine meniscectomies, especially for older patients with degenerative wear-and-tear injuries.
In a similar vein, a recent cross-sectional study published in PLOS One explores how meniscus injuries affect knee biomechanics, potentially exacerbating the risk of osteoarthritis when improperly managed. While surgical interventions were once the cornerstone of treatment paradigms, experts increasingly emphasize prevention, non-invasive alternatives, and judicious use of imaging technologies to avoid unnecessary procedures.
Beyond medical guidelines, this recalibration also reflects growing public demand for evidence-based care. Patients are asking tougher questions, and clinicians are under pressure to justify the benefits of invasive treatments. As one industry observer noted, “This is part of a larger trend—our understanding of orthopaedic medicine is becoming more nuanced, and blanket interventions are being replaced by tailored care.”

What Does This Mean for Patients?
For individuals living with knee pain or meniscus-related issues, these findings underline the importance of weighing options carefully and seeking second opinions. Knee injuries are notoriously complex, and quick fixes like surgery can sometimes create more problems than they solve. While surgical treatment may still be warranted for acute, sports-related tears in younger patients, many cases of degenerative meniscal damage may respond just as well—or better—to targeted physical therapy, lifestyle modifications, or pain management strategies.
Experts suggest that the decision to operate should be guided more by patient-centered outcomes—such as improvements in mobility, quality of life, and functional performance—than by the mere presence of a tear on an MRI scan. Conservative treatments, including personalized physiotherapy regimens, may often yield comparable results without the risks of surgical complications, post-operative pain, or delayed recovery times.
What’s Next? The Future of Knee Health
As the medical community comes to terms with these findings, the implications for patient care and healthcare policy are profound. More robust clinical guidelines may emerge, discouraging unnecessary surgeries except in narrowly defined cases. Research into preventative care and innovative therapies, such as biologics and regenerative medicine, will likely take center stage in efforts to address the knee health crisis without compromising outcomes.
In the meantime, patients are encouraged to stay informed, ask critical questions, and explore the full range of treatment options available. The study serves as a powerful reminder that surgery is not a cure-all, and less invasive paths often offer equally promising—and sometimes safer—routes to recovery.
The debate around partial meniscectomy highlights a broader truth about modern medicine: as technologies evolve and data accumulates, treatments must be reevaluated and updated to reflect the best possible evidence. For now, science urges both doctors and patients to tread carefully in treating meniscal injuries, keeping long-term outcomes at the forefront of decision-making.
The Takeaway
While knee surgery for cartilage damage has been a staple of orthopaedic care for decades, new evidence calls its efficacy into serious question. Patients and clinicians alike must weigh the benefits and risks of invasive treatments against non-surgical alternatives, prioritizing function and quality of life over outdated practices. As the field continues to evolve, one thing is clear: rethinking knee health is not just an option—it’s a necessity.